Why choose KGiS for insurance eligibility verification services?
Fast Approvals: Our real-time insurance eligibility verification services speed up patient admissions.
Accuracy Matters: With our detailed insurance verification services, we catch the smallest errors that can delay reimbursements.
Stay Updated: Navigating constantly changing insurance regulations can be tough. We keep you updated, ensuring continuous compliance and maximized reimbursements.
KG Invicta consistently delivers, guaranteed!
Verified
Insurances
5 Daysahead of appointment
Patient
Admission Improved
 31%
31%
95% of transactions
Turn around time
within
30 minLevel 1 Verification
A basic insurance eligibility verification process that focuses on coverage details of the patients as well as the co-pays and deductibles applicable.
Level 2 Verification
An in-depth verification process that involves gathering code-specific eligibility details with annual max or lifetime limits and authorizations, when required.
Insurance Eligibility Verification Process
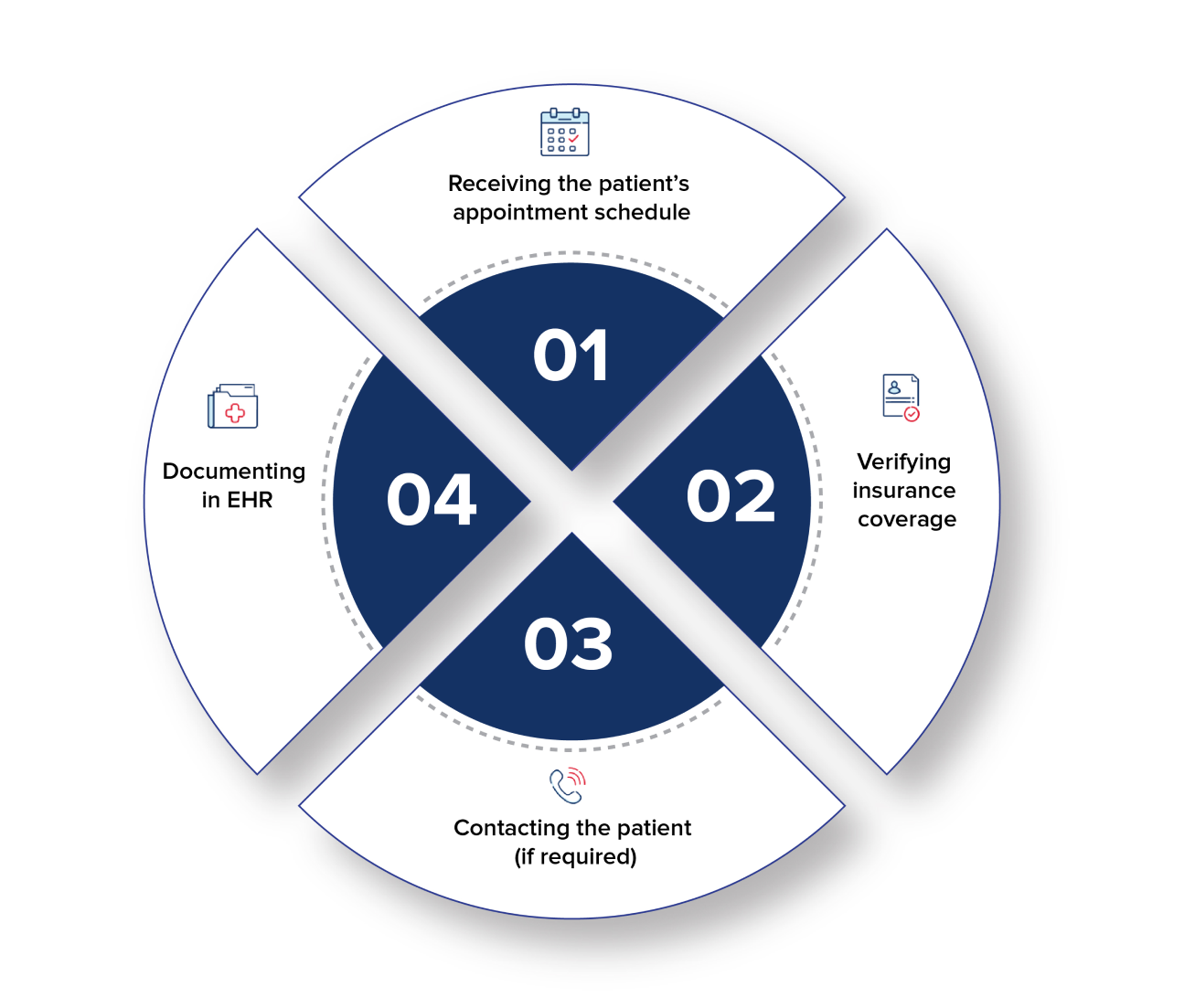
Partnering with KGiS means entrusting your insurance verification tasks to experts. Our skilled team collaborates directly with insurance providers to resolve any issues upfront, ensuring you’re prepared for every new patient who walks in.
Ready to make insurance verification effortless? Get in touch to find out how KGiS caters to all your needs, from Medicare verifications to confirming a patient’s insurance eligibility.











